How an old drug is coaxing new life into damaged brains
By Brad Hussey
Thanks to a chance discovery, an Ontario Institute of Regenerative Medicine (OIRM) research team is hot on the heels of a potential treatment for repairing damage to white matter in the brain — using a medication that is anything but new.
As you read this, your eyes are moving across the words on the screen while your brain translates the images into information you can comprehend. Perhaps one hand is slowly scrolling the page on your tablet screen, the other tasked with stirring your morning coffee. You tap your foot to today’s Spotify playlist.
These are simple acts most of us take for granted, the result of thousands of electronic messages being sent through your central nervous system (CNS; the brain and spinal cord) to the peripheral nervous system, which controls your limbs and organs. That the signals are successfully reaching their intended destinations means your nervous system is working well, thanks to an insulating layer of the brain and spinal cord called the myelin sheath. Myelin coats nerve fibres in the CNS to form white matter, which ensures those messages get where they need to go quickly, without short circuiting.
However, trauma and the effect of demyelinating diseases such as multiple sclerosis (MS) can damage white matter, resulting in diminished sensory, cognitive and motor function and a profound negative effect on quality of life and overall health. Millions of people live with some form of demyelinating illness, and brain injuries continue to be the leading cause of hospitalization, debilitation and death for children and youth. New treatments that correct white matter damage are therefore urgently needed.
Enter Dr. Freda Miller, senior scientist at Sick Kids Research Institute in Toronto, and collaborators at several Ontario institutions. Together, they are exploring potential approaches to stimulating stem cells in the brain to produce new oligodendrocytes, the cells that make up white matter, to restore brain function in children. Their ultimate goal: creating effective clinical therapies to treat brain injuries and neurological disease.
“We are focusing on children because their brains are still developing, which gives us two advantages,” Dr. Miller explains. “First, it means they have more stem cells in their brains to work with. Second, we need any new cells we produce to integrate into the circuits of the brain, and we reason that there is a greater chance in children for the new cells to become functional.”
Despite the cutting-edge science taking place in their Ontario labs, the team’s efforts focus in part on harnessing the potential of a medication widely used around the world for nearly 60 years. And unlike the neural messages traveling rapidly through your brain as you read, stir and tap your foot, the route the researchers took in identifying this approach is somewhat more circuitous.
The Science of Serendipity
Miller and her collaborators have long been interested in the idea that stem cells in the brain might be recruited to restore white matter. In 2010, their efforts focused on understanding the basic mechanisms underlying brain cell production. That research led to the unanticipated discovery of a pathway (aPKC-CBP) important for signaling stem cells in the embryonic brain to differentiate into both neurons and glial cells, including oligodendrocytes. Around the same time, Dr. Fredric Wondisford of Johns Hopkins University in Baltimore, MD coincidentally published research that observed the same pathway was activated in liver cells by metformin — a cheap, widely available generic medication introduced in 1957 to treat type 2 diabetes.
Jing Wang, at the time a post-doctoral research fellow in Miller’s lab and now a researcher at the Ottawa Hospital Research Institute, was then inspired to explore the possibility that the drug could be used to stimulate the production of new brain cells.
“We were enthusiastic about it, because if this was the case it would give us a very safe, accessible drug that could perhaps turn on stem cells in human brains and be used as a treatment for many different kinds of brain disorders,” Dr. Miller says. “Jing tested that idea and discovered that metformin could indeed turn on brain stem cells inside garden variety mice, and that it actually made them better at certain kinds of tasks that we know depend on new neurons being produced in the brain.”
Dr. Paul Frankland of the Hospital for Sick Children in Toronto, a neuroscientist and behavioural expert on the current OIRM project, was a co-investigator on this groundbreaking research, she adds.
More recent work led by neural stem cell expert Dr. Cindi Morshead of the University of Toronto — she’s also a member of the OIRM grant team — placed metformin in an even more compelling light. In research published last fall in Stem Cell Reports, young mice were given brain lesions to simulate the effects of pediatric stroke on motor and sensory functioning. When the mice were given metformin either through their mothers’ milk or through injection, they recovered and their symptoms resolved. Dr. Morshead and her co-authors concluded that treatment with metformin induced brain stem cells in the mice to differentiate and produce neurons and glial cells — in particular, the oligodendrocytes that make up white matter.
“Taken together, all of these results were very exciting. Originally we set out to learn how we could make new nerve cells, and here we were now able to make all kinds of new oligodendrocytes in mice,” Dr. Miller adds. “We said, ‘maybe this is going to be much more broadly applicable then we thought.’”
To test just how applicable, Dr. Miller is leading an OIRM-funded team in developing new approaches to measuring the impact of metformin in young people with white matter damage. They will also assess a combination of approaches to activate brain stem cells to produce oligodendrocytes, and hope to begin a metformin clinical trial in children and adolescents with white matter damage some time in 2017. Additional investigators include Drs. Morshead and Frankland, as well as Dr. Donald Mabbott, an expert in acquired brain injuries at the Hospital for Sick Children, Dr. Doug Munoz, director of the Centre for Neuroscience Studies at Queen’s University in Kingston, ON and neurologist Dr. Ann Yeh of Sick Kids Hospital.
“One of the things we are really thrilled about is how easily adoptable metformin will be as a clinical therapy if ultimately there is evidence that it works to repair white matter in humans. It will be a major step forward in treatment,” Dr. Miller enthuses. “And we’ve come this far all because of a serendipitous finding while pursuing basic science about how the brain is built and how it works.
“It’s a success story that highlights how Ontario is one of the hottest places in the world for stem cell research right now, and we’re excited to be a part of it.”
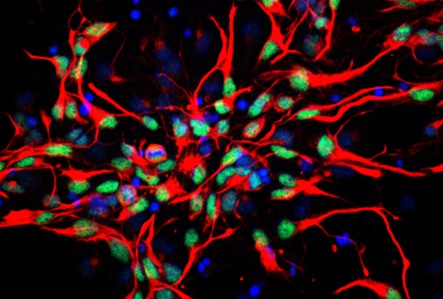
**Photo Credit: Cultured neural precursor cells from the developing mouse cortex. Photo courtesy of Dr. Freda Miller
