Solving a Burning Question
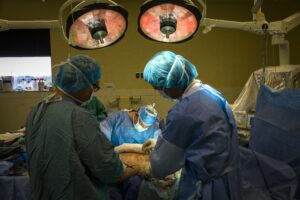 Sunnybrook researchers on a quest to improve wound healing using stem cells from patients’ own burned tissue
Sunnybrook researchers on a quest to improve wound healing using stem cells from patients’ own burned tissue
Each year, nearly half a million people are injured by burns requiring medical care in North America – as many as 3,000 are admitted to hospital annually in Canada alone. Beyond the pain and scarring associated with serious burns, these individuals face higher risk for lifelong recurring infection, potential loss of mobility and function, serious mental health impacts and a profound impact on quality of life.
Now, a Toronto-based research team hopes to change the long-term prognosis for burn patients by developing a skin substitute that utilizes stem cells culled from a patient’s burned tissue (autologous cells) to improve wound healing and scar quality while significantly reducing scar formation. Led by Dr. Marc Jeschke, medical director of the Ross Tilley Burn Centre at Sunnybrook Health Sciences Centre and senior scientist at the Sunnybrook Research Institute, the team has launched a phase 1 safety and efficacy trial in 12 patients with small burn areas of 5% to 20% of their total body surface area (TBSA). If their approach is deemed safe and effective, a second phase of 12 patients with TBSA burns of greater than 20% will proceed.
The trial is supported by a $450,000 Disease Team grant from the Ontario Institute for Regenerative Medicine, as well as funding contributed by Toronto Hydro and the Sunnybrook AFP Innovation Fund.
“This is the first clinical trial using autologous cells to treat burns by extracting and processing mesenchymal stem cells from burnt skin, which is normally discarded in surgery,” Dr. Jeschke says. “We found in large animal trials that the approach has a significant impact, not only on healing speed, but also on scarring. In those trials, wounds look tremendously better as compared with controls. Our hope is that this can be translated into humans.”
Here’s how the proposed treatment works: First, burned tissue is surgically removed from a patient. Next, mesenchymal stem cells (which can differentiate into muscle, bone, cartilage, fat cells and more) are collected from that tissue. Those cells are then infused into an existing wound dressing called Integra®, a sort of scaffold applied as a thin sheet that enables cells and capillaries to grow and heal the wound – in effect, creating transplantable sheets of the patient’s skin.
“Because we are using the patient’s own cells, we overcome the problem of immune reactions when using skin grafts using tissue from healthy donors,” Dr. Jeschke continues. “A burn patient is at significantly increased risk for sepsis and organ failure, and so avoiding the need for immunosuppressants is incredibly beneficial.
The process will also enable physicians to avoid having to transplant the patient’s healthy skin onto burned areas, which just creates more potential problems – if they have TBSA burns of 30%, another equal amount of skin would be required to create the grafts.
Beyond the potential impact for burn patients, Dr. Jeschke adds that the treatment could also mean reduced need for surgeries and shortened hospital stays, resulting in significant savings for health systems.
“Burn patients deserve a reliable treatment that accelerates healing and reduces scarring and other long-term effects,” Dr. Jeschke concludes. “I think we will learn a lot from this trial. It’s a first step toward what could be a game-changing approach.
“I don’t think we could have done this trial anywhere else in the world but here in Ontario, given its stem cell research and commercialization infrastructure, including the knowledge and the drive for innovation that’s here. It’s quite unique – I’m still here because you can’t find this anywhere else in the world.”
