Timing is everything for premature babies and their developing gut
By Meredith Hanel
An intestinal disease among newborns with a mortality rate of 30 per cent has Dr. Tae-Hee Kim seeking links between gut stem cells and microbiota.
When Archimedes famously linked the word “Eureka” with a scientific discovery — in this case volume displacement — his excitement was so great that he purportedly ran naked through the streets of Syracuse to share his finding. Few scientists today would venture unclothed to relay their own eureka moment, but that doesn’t mean the excitement of discovery is any less.
For a mouse geneticist, that eureka moment is creating a phenotype: the physical manifestation of a genetic change. Double eureka if that phenotype matches a human condition.
In Toronto, SickKids researcher and OIRM PI, Dr. Tae-Hee Kim has found just that: “We just saw this cool phenotype a couple of weeks ago. We think we have a genetic model resembling NEC symptoms.” Kim is excited, but cautious, as it’s still early days.
NEC is short for necrotizing enterocolitis, a neonatal inflammatory disease that ravages the intestines, with a mortality rate as high as 30 per cent. Preemies are more susceptible to NEC and scientists think something about postnatal intestinal maturation is going awry. With the earlier shift from the womb to the outside world, perhaps intestinal cells don’t get the right signals at the right time.
Adjusting to a completely different environment outside the womb, the intestine, a protective barrier, must quickly tighten the border between the inside body and outside world. Postnatal intestines need to absorb nutrients but keep out harmful microbes and toxins. The intestinal surface will be colonized by a host of new microbes it has never seen before. Signals running between microbes and the gut are thought to be part of the process of intestinal maturation that takes place after birth.
“The gut microbiota is critical we think for intestinal development and stem cell development and we are actually investigating this question,” says Kim, which is why his postdoc Dr. Ji-Eun Kim, a veterinarian scientist, is researching how microbiota impact intestinal stem cells and immune system development to better understand NEC.
Intestinal stem cells don’t develop until after birth and earlier birth could affect the signals that control their development. Kim’s mouse research shows that the timing of intestinal stem cell specification coincides with the onset of induced NEC. Other researchers have induced NEC in mice with a series of stresses and conditions including premature birth. Kim’s lab suspects that NEC begins in defective intestinal stem cells. To test this theory Kim’s team made mice with defective intestinal stem cells by knocking out a gene postnatally that is critical for intestinal stem cell development, hoping it would cause NEC symptoms. It did and that’s what this “cool phenotype” is all about.
In addition to the stem cell differentiation defect they were expecting, they see NEC-like symptoms such as spontaneous inflammation, cell death and signs the intestine is attempting to regenerate. They are working on verifying that the symptoms are similar enough to NEC in humans to make it a good model to understand the disease progression. Postdoc Dr. Sabrina Coquenlorge-Gallon in the lab brings her experience working on inflammatory bowel disease to understand the inflammation occurring in these NEC-like mice.
A fluorescent protein marks the intestinal stem cells of the NEC-like mice and is used to capture them. The team plans to compare these defective stem cells with unaltered mouse intestinal stem cells to see which genes and proteins are turned on or off differently. Eventually, they hope to pinpoint differences between molecular signatures for normal stem cells and defective stem cells associated with NEC. Some of these differences might also be found in humans and turn out to be early screening markers for NEC, better than current NEC biomarkers that are immune-related and may detect the disease too late. “If we can identify the markers when there is no obvious inflammation, but showing some stem cell genes abnormally expressed, these markers might be much more effective,” explains Kim.
“If we can restore normal stem cell function, then these stem cells will repopulate the entire lining and we might be able to reduce NEC symptoms.”
Of all the stem cells maintaining our body, intestinal stem cells are the busiest. Covered with tiny finger-like protrusions called villi, the surface area of our intestinal lining is actually about the size of half a badminton court. It’s also a surface that is constantly regenerating: every 3–5 days as it is repopulated with entirely new cells. “For me this is an amazing self-renewing organ to study stem cell mechanisms,” says Kim.
Dr. Kim always wanted to study human disease and pursued cancer research during his training but finds it funny that, “I ended up studying developmental biology all the time.” Now things have come full circle because his expertise on the normal function of genes and proteins and the sequence of events in intestinal development give him an excellent vantage point to see what goes wrong in diseases like cancer, inflammation and NEC. Being awarded an OIRM New Ideas grant gave his lab a chance to investigate their hypothesis that NEC begins with a stem cell defect. “In my lab we are basic scientists, we study fundamentally basic questions about how gut stem cells are specified but this grant allowed us to expand our research program to include studying basic mechanisms of diseases, critical deadly diseases such as NEC,” says Kim.
Many of Kim’s collaborators are also at SickKids, like developmental biologists Dr. Chi-Chung Hui and Dr. Janet Rossant, former OIRM president. To apply the findings from his mouse work to human cells, Kim will work with Dr. Augostino Pierro, a leading clinician scientist in the NEC field. Kim appreciates the wealth of expertise and resources found in Toronto, like the world-class mouse facility, The Centre for Phenogenomics, and says, “Many people here study stem cells and many bioengineers and chemists are collaborating with stem cell researchers to do more interdisciplinary research and I really love that kind of research environment.”
Assembling the right team will be just as important as Kim brings his research forward. Once his team verifies that their “eureka” mouse is, in fact, a solid phenotype for NEC, the next step will be to design treatments to repair intestinal stem cells in their mice. From there, the team plans to use human organoids — miniature organ-like structures made from cultured cells from NEC patients — to further test out these treatments. If all goes according to plan, there will be many more eureka moments in the Kim lab in the years to come.
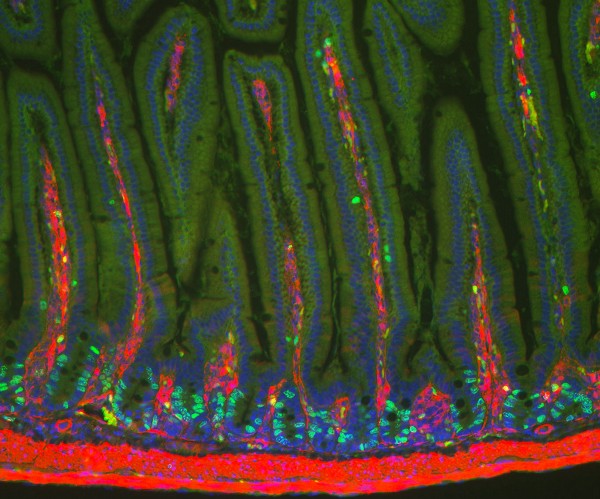
**Photo courtesy of Dr. Tae-Hee Kim showing intestinal villi. Stem cells are located in the crypts where proliferating cells are labelled bright green.
